INTRODUCTION
Modern restorative dentistry has evolved towards aesthetically advanced materials, seeking excellent color stability and adhesion to dental tissues whether bonding to enamel or dentin, depending on the case. 1 This includes resin cements, which have become the preferred option for the cementation of indirect restorations including veneers, inlays, and metal-free crowns due to their strong adhesive properties and mechanical stability. 1 However, discoloration over time is a significant concern, as it compromises the aesthetics of the restoration. 1
The color change in resin cements is attributed to various internal and external factors. 1 Tertiary amines used in dual-cure and chemically activated polymerization systems have been identified as a key factor in color alteration. 2 In response, amine-free resin cements have been developed to mitigate this effect and improve color stability particularly in thin restorations, where discoloration is more perceptible. 2 This article aims to evaluate the factors influencing the color stability of these cements and explore the methods used for their assessment. 3
TYPES OF RESINS CEMENTS
Resin cements are essential materials in restorative dentistry, used to bond indirect restorations such as crowns, bridges, onlays, inlays, and veneers. 3 Their composition is based on an organic matrix of monomers, such as Bis-GMA (bisphenol A glycidyl methacrylate) or UDMA (urethane dimethacrylate), combined with inorganic fillers that enhance mechanical strength and dimensional stability. 3 The classification of resin cements is primarily based on their polymerization mechanism and adhesive properties. The main types are described below. 3
LIGHT-CURED RESIN CEMENTS.
These cements polymerize through exposure to a light source, typically in the blue spectrum, which activates photoinitiators, such as camphorquinone present in their composition. 4 This activation induces the formation of free radicals that initiate the polymerization of the material. 4 One of the most notable advantages of light-cured cements is the control over working time, as polymerization does not begin until the light is applied, allowing for precise placement of the restoration; however, their use is limited to situations where light can adequately penetrate, such as in thin and translucent restorations, for example, porcelain veneers or ceramic restorations with a thickness of less than 0.6 mm. 4 Additionally, these cements offer excellent color stability and favorable mechanical properties, such as high hardness and wear resistance. 4 However, their application in areas where light cannot reach properly may result in incomplete polymerization, compromising the integrity of the restoration. 5
SELF-CURED RESIN CEMENTS.Also known as chemically cured cements, these materials polymerize without the need for light through a chemical reaction between two components: a base containing aromatic tertiary amines and a catalyst containing benzoyl peroxide. When mixed, a redox reaction initiates the polymerization of the material. This is a type of chemical reaction in which an electron transfer occurs between two substances; it is called 'redox' because it involves both reduction and oxidation simultaneously, which triggers the polymerization of the material. 5 They are ideal for situations where light cannot penetrate, such as the cementation of metal restorations, metal-ceramic restorations, or endodontic posts. 5 However, they have some disadvantages, including a shorter working time and lower color stability due to the oxidation of amines, which can affect long-term aesthetics. 5 Additionally, removing excess cement can be more challenging once the material has fully set. 4
DUAL-CURE RESIN CEMENTS.
These cements combine both chemical and light-curing polymerization mechanisms as they contain both photo initiators and chemical initiators, allowing them to polymerize initially through light exposure and continue polymerization chemically in areas where light cannot reach. 6 This dual mechanism makes them versatile and suitable for a wide range of clinical applications, including the cementation of thick or opaque restorations where light penetration is limited. However, studies have shown that chemical activation alone may not be sufficient to achieve optimal polymerization, therefore, it is recommended to supplement with light curing whenever possible to ensure the best mechanical properties and adhesion. 4
SELF-ADHESIVE RESIN CEMENTS.
These cements have been developed to simplify the cementation process by eliminating the need for a separate adhesive system. 6 They contain acidic monomers that simultaneously demineralize and adhere to the dental structure, allowing for direct chemical adhesion to enamel and dentin. 6 They offer easier handling and reduce clinical time, as they do not require additional steps such as acid etching or adhesive application. However, their adhesive strength may be lower compared to cements that use conventional adhesive systems, and their color stability may be compromised over time. 5 Self-adhesive resin cements are suitable for the cementation of restorations where maximum adhesive strength is not critical and when a more simplified technique is desired. 6
FACTORS INFLUENCING THE COLOR CHANGE OF RESIN CEMENTS
Ceramic veneers have revolutionized aesthetic dentistry, enabling conservative restorations with highly satisfactory results; however, selecting the appropriate resin cement is crucial to ensuring color stability and long-term durability of the restoration. 6 Various studies have investigated the impact of different brands, shades, and polymerization modes of resin cements on the appearance and strength of ceramic veneers. 7
INTERNAL FACTORS
The chemical composition of resin cements directly influences their color stability. 7 The organic matrix consists of monomers such as Bis-GMA, UDMA, and TEGDMA. The proportion and type of monomers determine water absorption, resistance to degradation, and consequently, chromatic stability. 4
The inorganic matrix consists of filler particles such as silica, barium glass, and zirconium oxide. These particles not only enhance the mechanical properties of the cement but also affect its response to light and interaction with external agents. 7
The organic matrix
The organic matrix of resin cements is primarily composed of methacrylic monomers, which directly influences the material's stability, mechanical strength, and behavior regarding water absorption and external pigmentation. The most commonly used monomers include: 7
Bis-GMA (Bisphenol A-Glycidyl Methacrylate): One of the main components of the organic matrix due to its high viscosity and excellent mechanical properties. 7 Its relatively large molecular structure and intermolecular hydrogen bonds provide rigidity and mechanical strength; however, due to its hydrophilic nature, it tends to absorb water over time, which can cause material swelling and changes in color stability. 8 Water absorption may also weaken the matrix and reduce its durability. 8
UDMA (Urethane Dimethacrylate): Less viscous than Bis-GMA, with a chemical structure that results in lower water absorption. Due to its lower hydroxyl group content, it offers better color stability and higher resistance to hydrolytic degradation. 8 It is used in formulations where lower rigidity and greater material flowability are required. 8
TEGDMA (Triethylene Glycol Dimethacrylate): Functions as a diluent, reducing the cement’s viscosity to facilitate handling and clinical adaptability; however, its highly hydrophilic nature makes it more susceptible to water absorption and pigmentation over time, potentially compromising the cement’s color stability. 8 Additionally, its lower molecular weight increases polymerization shrinkage, which can create internal stresses and affect the adhesion of the resin cement. 8
The combination of these monomers in appropriate proportions allows for a balance between mechanical strength, viscosity, and color stability in resin cements. Generally, formulations with lower TEGDMA content and a higher proportion of UDMA tend to exhibit better performance against water absorption and external pigmentation. 8
The Inorganic matrix
The inorganic matrix of resin cements is composed of filler particles that significantly impact the material's optical, mechanical, and color stability properties. These particles include: 9
Colloidal Silica: Used to enhance mechanical strength and material stability. Its nanometric-sized particles help increase light dispersion and improve the cement's translucency, contributing to a more natural aesthetic effect. Additionally, its incorporation reduces porosity, decreasing the absorption of external pigments. 10
Barium Glass: Provides radiopacity to the material, facilitating its detection in radiographs. Its size and distribution affect the translucency and refractive index of the cement. Cements with finer barium glass particles tend to exhibit better color stability and lower water absorption. 10
Zirconia (ZrO2): Incorporated to improve the mechanical strength and durability of the cement. Zirconia also helps reduce surface degradation and the absorption of external pigments. 10 Due to its high refractive index, it also influences the aesthetic appearance of the cement, particularly its ability to blend with the dental structure. 11
Particle Size and Distribution: Nanometric fillers improve light dispersion, reducing the impact of external pigmentation. 11
Refractive Index: Compatibility between the refractive index of the organic matrix and the inorganic filler enhances the optical stability of the cement. 11
Cements with a high filler content and smaller particles tend to be more resistant to color changes, as they absorb less water and exhibit less surface degradation. 11
EXTERNAL FACTORS
Exposure to coloring substances is a key factor in the color change of resin cements. 11 Beverages such as coffee, red wine, and Coca-Cola have been shown to be highly pigmented, especially in materials with high surface porosity. 12 Additionally, the surface roughness of the cement influences the amount of pigment absorbed. 12
The humidity of the oral environment, temperature, and pH also play an important role, as they can promote hydrolysis or surface degradation processes. 12 In addition, the clinical technique used for light curing (light intensity, exposure time, type of lamp) can affect the degree of conversion and, consequently, the long-term color stability. 12 Polymerization is another crucial aspect of color stability. 11 Dual-cure and self-cure cements tend to discolor more due to the oxidation of tertiary amines. 13 In contrast, light-cured cements, which lack co-initiators, exhibit greater color stability. 13
PHOTOPOLYMERIZATION AND MICROHARDNESS OF RESIN CEMENT
The quality of the resin cement light curing process is a key factor that directly influences its mechanical properties, especially its strength and adhesion capacity to the dental structure. 13
Several studies have shown that insufficient polymerization, particularly when using reduced light exposure times, can negatively affect the material’s surface hardness. 13 This decrease in microhardness compromises both dimensional stability and the effectiveness of adhesive sealing, essential factors for the clinical longevity of restorations; however, despite variations in light-curing protocols, some analyses have not shown statistically significant differences between the hardness of the upper surface (closer to the light source) and the lower surface (further away), suggesting that certain resin cements may exhibit relatively uniform polymerization under specific exposure conditions. 13
SPECTROPHOTOMETER, AS A METHOD FOR EVALUATING COLOR CHANGE
The spectrophotometer in dentistry is a tool used to measure the color of teeth and dental materials with high precision and objectivity. 14 Its operation is based on the emission of a light source onto the surface of the tooth or restorative material and the measurement of the amount of light reflected at different wavelengths. 14 From this information, the device generates numerical values that represent the color according to standardized systems, such as the CIE Lab®. 15
OPERATION OF THE SPECTROPHOTOMETER IN DENTISTRY
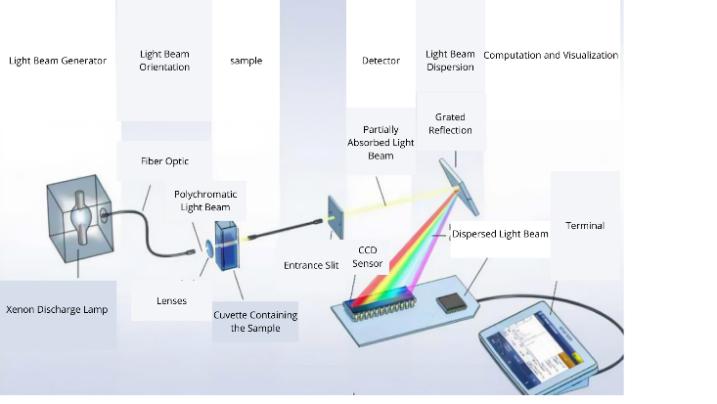
The spectrophotometer emits a beam of white light or a specific range of wavelengths onto the dental or restorative surface. Some of the light is absorbed, while the rest is reflected. 15 The amount and type of reflected light depend on the color and translucency of the evaluated material, a sensor in the spectrophotometer detects the reflected light and breaks it down into different wavelengths. 14 These values are compared with a color database to determine the exact color of the tooth or restorative material. 14
The CIE Lab® system is the most commonly used in color stability studies. 14 The CIE Lab® method allows for precise quantification of color differences using the ΔE (color difference) formula, where higher values indicate more perceptible color changes. 15
This system evaluates the following parameters:
L*: Lightness (0=black, 100=white)
a*: Red-green dimension (positive values indicate red; negative values indicate green.)
b*: Yellow-blue dimension (yellow indicates positive values, blue indicates negative values). 15
However, to properly interpret the results obtained, it is essential to consider technical aspects that can affect the accuracy and reliability of the measurements. One of the determining factors is the calibration of the spectrophotometer, which must be performed regularly according to the manufacturer's specifications. Poor calibration can lead to inaccurate or inconsistent measurements. 15 In addition, environmental conditions such as temperature, relative humidity, and especially the lighting in the surroundings during the measurement, can alter the perception and capture of color, even in automatic devices. 15
The margin of error of the spectrophotometer may vary depending on the model and the sensitivity of the sensor, but in clinical or laboratory applications, a standard deviation of less than 1 ΔE unit is expected to ensure accuracy; however, studies have shown that values close to the threshold of visual perception (ΔE ≈ 1.0 to 3.3, depending on the context) can be difficult to interpret if these variables are not carefully controlled. 14
The type of material surface (porosity, texture, gloss) should also be considered, as these characteristics affect the light reflectance and, therefore, the color reading. 15 For this reason, it is recommended to perform measurements on polished and homogeneous surfaces, standardizing both the sensor distance and the angle of light incidence. 14
CLINICAL IMPLICATIONS OF AMINE-FREE CEMENTS
Amine-free resin cements have shown greater color stability compared to conventional cements; however, their bond strength may be compromised if proper adhesion protocols are not followed. 15 The use of compatible adhesive systems and prolonged photopolymerization is recommended to optimize their performance. 10 Additionally, the selection of the type of restoration influences the effectiveness of these cements. 11
Thicker restorations provide greater protection against the absorption of external pigments, while thin veneers may allow greater translucency of the cement, affecting the final color of the restoration. Therefore, color changes should not be attributed solely to resin cements; other factors must also be considered, such as the type of restoration, the pigments to which the restoration will be exposed in the oral environment, the type of adhesion, and proper photopolymerization, among others. 1 , 15
CLINICAL WARNINGS ABOUT AMINE-FREE RESIN CEMENTS
Slower or Incomplete Polymerization: Due to the absence of amines, these cements may exhibit slower or less efficient curing kinetics under certain light conditions, potentially affecting the degree of conversion and final strength.¹¹
Compatibility with Curing Lights: It is essential to ensure that the curing light used emits within the appropriate spectrum to activate the alternative photoinitiator system (e.g., Ivocerin, TPO, or Lucirin TPO-L), as these do not react the same way as camphorquinone/amine-based systems.¹¹
Technique Sensitivity: Some amine-free systems may require stricter control over the curing time and light intensity, demanding precision in the clinical protocol.¹¹
Interaction with Adhesives: These cements may be incompatible with certain adhesive systems, especially those containing residual amines or components that interfere with the alternative photoinitiator.¹²
Limited Working Time: When using self-curing systems without amines, working time may be shorter or less predictable, depending on the manufacturer.¹¹
Evaluate Color Stability: Although amine-free cements offer better long-term color stability, it is important to confirm this with clinical data for the specific product and to avoid exposure to contaminants that may alter the color. 15
Cost and Availability: They are usually more expensive and less widely available, so a cost-benefit analysis should be conducted for each clinical case.¹¹
CONCLUSIONS
Amine-free resin cements represent an innovation in modern dentistry, offering better color stability compared to traditional resin cements. Internal factors, such as the composition of the matrix, and external factors, such as exposure to pigments, play a significant role in the aesthetics of restorations cemented with these materials. Therefore, by following a proper cementation protocol, considering adhesion and polymerization, we can ensure good color stability and excellent mechanical strength, thus meeting the demands of modern dentistry.
References
- Pissaia JF de Almeida Guanaes BK de Almeida Kintopp CC Correr GM Fernandes da Cunha L Castiglia Gonzaga C Color stability of ceramic veneers as a function of resin cement curing mode and shade: 3-year follow-up PLoS One 2019 14 7 e0219812
- Heboyan A Vardanyan A Karobari MI Marya A Avagyan T Tebyaniyan H Dental luting cements: an updated comprehensive review Molecules 2023 28 4 1619
- Yang Y Wang Y Yang H Chen Y Huang C Effect of aging on color stability and bond strength of dual-cured resin cement with amine or amine-free self-initiators Dent. Mater. J. 2022 41 1 17 26
- Albaheli BI Elawsya ME Ali AI Microleakage of lithium disilicate veneers bonded to different substrates with light-cure and dual-cure resin cements J. Clin. Exp. Dent. 2024 16 4 e431 9
- Zhou W Liao ZX Chen JH Qiu BY Zhang Y Zhang L Color change of glass ceramic restorations cemented by four types of dual-cured resin luting agents with different initiator systems Dent. Mater. J. 2022 41 6 833 42
- Huang W Ren L Cheng Y Xu M Luo W Zhan D Evaluation of the color stability, water sorption, and solubility of current resin composites Materials 2022 15 19 6710
- Santos M Fidalgo-Pereira R Torres O Carvalho O Henriques B Özcan M The impact of inorganic fillers, organic content, and polymerization mode on the degree of conversion of monomers in resin-matrix cements for restorative dentistry: a scoping review Clin. Oral Investig. 2024 28 8 454
- Fidalgo-Pereira R Torres O Carvalho Ó Silva FS Catarino SO Özcan M A scoping review on the polymerization of resin-matrix cements used in restorative dentistry Materials (Basel) 2023 16 4 1560
- Ferracane JL A historical perspective on dental composite restorative materials J. Funct. Biomater. 2024 15 7 173
- Tabatabaei MH Matinfard F Ahmadi E Omrani LR Mahounak FS Color stability of ceramic veneers cemented with self-adhesive cements after accelerated aging Front. Dent. 2019 16 5 393 401
- Meleka NM El-Banna A El-Korashy DI Color stability and degree of conversion of amine-free dual-cured resin cement used with two different translucencies of lithium disilicate ceramics Braz. Dent. Sci. 2023 26 2 e3614
- Lei MA Macchi RL Picca M Effect of photopolymerization time on the microhardness of resin cement beneath feldspathic ceramic Acta Odontol. Latinoam. 2023 36 1 40 6
- Hickel R Mesinger S Opdam N Loomans B Frankenberger R Cadenaro M Revised FDI criteria for evaluating direct and indirect dental restoration recommendations for its clinical use, interpretation, and reporting Clin. Oral Investig. 2023 27 6 2573 92
- Reyes-Angeles MC Cuevas-Suárez CE Trejo-Carbajal N Herrera-González AM Rivera Gonzaga JA Evaluation of novel fluorescent 1,5-naphthalene-bis(allylcarbonate) monomer used in the formulation of dental composite resins Polym. Bull. 2024 81 9 8159 76
- Crespo PC Córdova AK Palacios A Astudillo D Delgado B Variability in tooth color selection by different spectrophotometers: A Systematic Review Open Dent. J. 2022 16 e187421062211180
